Providing seating interventions for individuals with very complex impairments can be quite challenging. One of the tools available to address complex needs is custom contoured seating.
Many years ago, this approach was born of orthotic approaches that emphasized “total contact” to provide both postural control and pressure distribution.
As with any other seating intervention, the decision to use custom contoured seating begins with a thorough evaluation by the clinical team. The Mat evaluation allows the team to determine the limitations of movement that need to be accommodated, and the level of support needed. This is also the time that realistic support goals begin to be created. For example, there is a difference between “lifting” a trunk and supporting a trunk. We cannot lift and correct, we support. Orthotists are trained to provide that kind of correction through the use of circumferential supports such as TLSO (thoraco-lumbar-sacral supports- “body jackets”). This then leads to positioning goals that are used to inform the actual molding. Without these steps, the molding ends up being a process of making shapes without regard to client need.
When is custom-contoured seating appropriate? It is not a method that should be taken lightly, it does require a certain degree of learning the method and practice with that method. Often, the manufacturer’s representative can assist the clinical team with learning the method of molding. Some manufacturers have classes in which they provide hands on guided practice. It is important to recognize and understand those different methods of molding and manufacturing the seat and/or back components that mold, have different outcomes in terms of comfort, support characteristics and ability to modify for growth and change. The clinical team must understand this in order to have a successful match to the client.
Custom contoured seating can be used with such impairments as multiple plane asymmetries (i.e., pelvic rotation, obliquity, scoliosis, kyphosis occurring at the same time), collapsing asymmetries and movement disorders.
Once it is determined that molding may be a useful intervention for a client, it must be trialed to assess the effect on tolerance and function. Some clients can adapt to total contact and some cannot. Some clients have very specific patterns or ways that they must move to achieve function. There can be unintended consequences of this type of support. Some examples include:
- Decreasing micro-movements that clients use for function, such as can be seen with Muscular Dystrophy or high spinal cord injuries. These movements, which may not be very apparent, can relate to achieving function and comfort.
- Over-supporting an individual with a movement disorder. Some of these movements may seem asymmetrical and inappropriate at first site, but these patterns are often needed to achieve function.
Some methods allow the client to be molded in in their equipment, or equipment that is similar. This can be especially important if the clinical team wishes to maintain or facilitate function, such as driving a powered chair or accessing vehicle driver controls. The time to discover whether or not the custom contoured seating works is not at the delivery/fitting.
In summary, custom contoured seating is a powerful tool in the clinical team’s toolbox. Things to keep in mind:
- Ensure there are a complete set of linear and relative body angular measures at the evaluation that are then compared at the time of fitting
- Know your seating goals
- Everything has to be in place prior to molding, foot, upper extremity, head support, etc., otherwise you will end up with a mold that doesn’t fit or have the shapes that you intended.
- Quality of outcome = quality of preparation
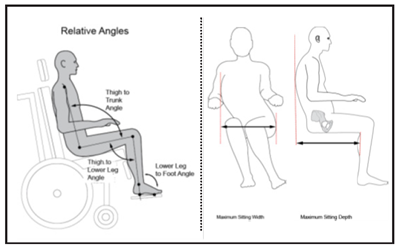
These are angular measures and additional linear measurements that are useful to record during the mat eval process (2)

author
Susan Johnson Taylor
OTR/L
Susan Johnson Taylor is an occupational therapist who has been practicing in the field of seating and wheeled mobility for 40 years primarily in the Chicago area at the Rehabilitation Institute of Chicago Wheelchair and Seating Center (now the Shirley Ryan Ability Lab). Susan has published and presented nationally and internationally and has consulted on product development for a variety of manufacturers. Susan is both a member and fellow with RESNA. She is currently a member of the Resna/ANSI Wheelchair Standards Committee and the Clinician’s Task Force. She is a Certified member of the International Society of Wheelchair Professionals.



